Other links or resources
Read related stories
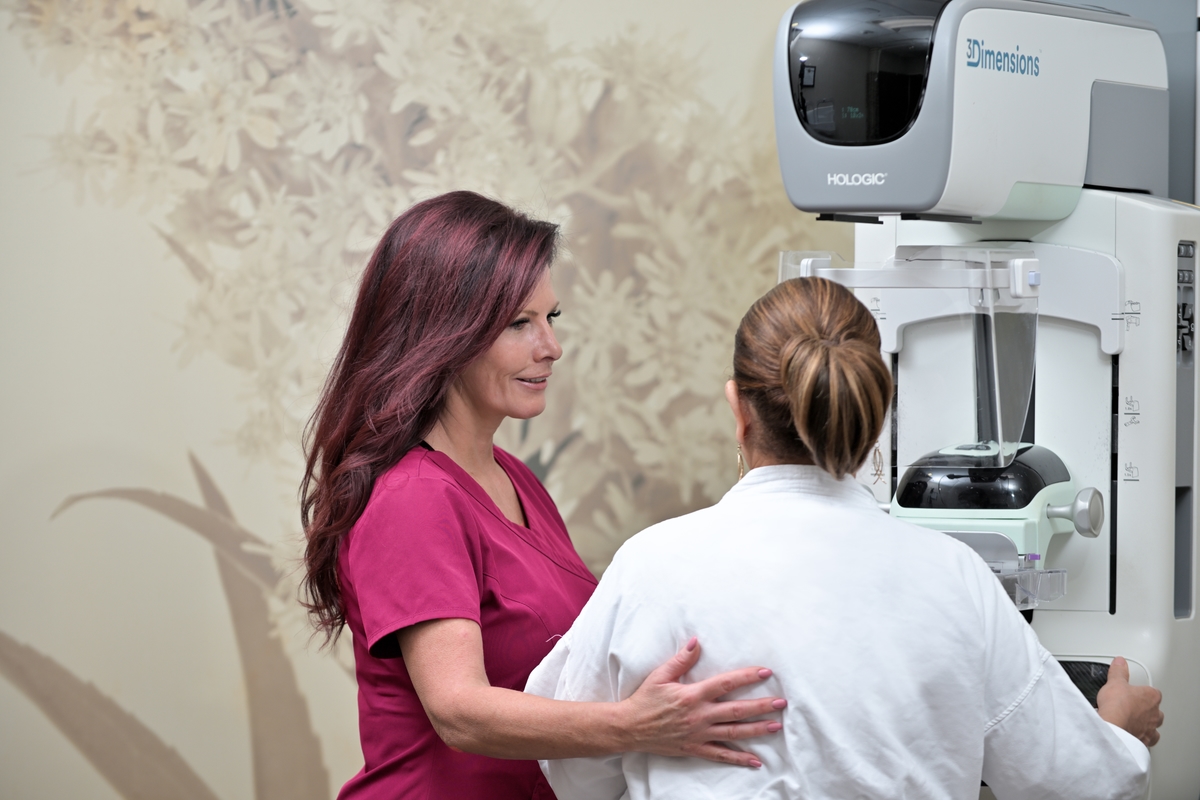 Consumer Health
Consumer HealthConfused About Breast Cancer Screening? Here’s What Doctors Want You to Know
When it comes to breast cancer screening, the advice can feel all over the place—start at 40, no, 45. Get a mammogram every year, or maybe every two. Add an ultrasound if your breasts are dense. Consider an MRI if you’re high-risk.
It’s no surprise so many women are left wondering: what’s right for me?
To help cut through the confusion, we’ve put together a guide to explain the different types of breast cancer screening, when they’re recommended, and how to know which one is right for you.
Know Your Risk
Before scheduling your first mammogram, take a moment to learn where you stand. The American College of Radiology and the American Society of Breast Surgeons recommend that all women have a breast cancer risk assessment by age 25.
This conversation with your doctor starts with a detailed personal and family history. From there, risk models can help identify women who may be more likely to develop breast cancer—and who might benefit from earlier or more frequent screening.
Knowing your risk gives you a roadmap: when to begin screening, how often to go, and whether extra imaging—like ultrasound or MRI—should be part of your plan.
Explore Your Screening Options
Mammogram: The Gold Standard
A screening mammogram is recommended every year for women of average risk beginning at age 40. Women at higher risk may need to start mammograms sooner.
A mammogram is a low-dose X-ray that can spot small changes in breast tissue—often years before symptoms arise. It’s fast, safe, and remains the gold standard for early detection, when treatment is most effective.
“During a mammogram, you’ll feel some pressure as the breast is gently compressed,” explained Mindy Goldfischer, MD, chief of breast imaging and medical director of The Leslie Simon Breast Care and Cytodiagnosis Center at Englewood Health. “That compression is what allows us to get the clearest, most accurate images while keeping radiation exposure low. It only lasts a few seconds—and that brief pressure can make all the difference in detecting an early cancer.”
Ultrasound: Added Clarity for Dense Breasts
Sometimes a mammogram needs backup. If you have dense breast tissue, which can make mammograms harder to read, your doctor might recommend an annual ultrasound in addition to your mammogram. Dense tissue is more common in younger women, but it can occur at any age. Not sure if you have dense breasts? Under federal law, all mammogram reports must include this information.
Ultrasound can also be used to learn more about a finding detected on your mammogram—helping determine whether a suspicious area is a lymph node, cyst (a noncancerous, fluid-filled pocket), or solid tissue that may require a biopsy.
MRI: A Deeper Look for High-Risk Women
An MRI uses magnets and radio waves (not X-rays) to create detailed images of the breast. After a contrast dye is given, areas of abnormal blood flow stand out more clearly—helping to identify even very small changes.
MRI is used alongside mammography, not in place of it, because each test can reveal different types of abnormalities. Together, they provide the most complete picture.
Because MRI is extremely sensitive, it sometimes detects things that are not cancer but may need additional evaluation. That is why MRI is generally reserved for women who truly need that level of detail. For women at higher risk—such as those with certain genetic mutations or a strong family history—it can offer meaningful added reassurance.
Why Not Just Do Them All?
It can be tempting to want every test available, but more imaging doesn’t always mean better care.
“Unnecessary tests can sometimes lead to anxiety, false positives, and even follow-up procedures that may not be necessary and do more harm than good,” Dr. Goldfischer said. “That’s why a personalized plan—based on your age, risk, and breast density—is the safest and most effective way to screen for of breast cancer.”
It’s also important to stay familiar with how your breasts normally look and feel. This isn’t about doing a structured monthly exam, but about understanding your own baseline, so you can recognize any new changes—like a lump, thickening, pain, or skin differences—and share them with your doctor right away.
The Bottom Line
Early detection saves lives—and the right screening makes all the difference. Don’t let confusion stop you or wait for symptoms to arise before taking the next step. Schedule your screening, ask questions, and stay proactive about your breast health.
Posted November 17, 2025